This story is part of our Rainbow Rewind 2019 series—looking back at the past year and decade in politics, health, culture and more.
We made it through another year! It’s been a difficult one for our mental health and well-being. U.S. President Donald Trump is quite literally stressing people out: One Pew Research Center study reported that Trump’s comments and statements make Americans feel (in this order): concerned, confused, embarrassed, exhausted, angry, insulted and frightened. Our warming planet is affecting our physical health through poor air quality, housing and food insecurity—it’s also taking a toll on our mental health, with climate change-related conditions such as post-traumatic stress disorder, depression, anxiety, grief and substance use disorders. But the headlines aren’t all bad: This year we’ve also made significant strides—and new discoveries—in LGBTQ2 health.
From a ground-breaking federal report on the health of LGBTQ2 Canadians to new rules on sperm donation to insight into the well-being of Two-Spirit, Black and bisexual people’s health, this year has shown that there’s so much to learn about our communities, and still so much to be done.
Here are some of the top stories in LGBTQ2 health this year.

New global guidelines released on providing care to trans patients
One of the world’s largest medical journals has published recommendations for providing effective care to transgender patients. Last year, a small study suggested that while most healthcare providers in the U.S. are willing to provide routine care to trans patients, they lack the training to effectively care for trans individuals. Care of the Transgender Patient provides guidance to physicians through various facets of care, like defining and using correct terminologies about a patient’s gender identity, understanding hormone therapy and trans-specific surgeries as well as the legal issues involved in the care of trans people.
Health Canada will change sperm donation rules
Come one, come all! Canada hasn’t been the most welcoming to sperm donors, especially gay ones—but that’s going to change next year.
Almost all donor sperm in Canada is imported from the U.S.—and even then, the country only has a few hundred donors. Why? Sperm safety regulations in Canada are quite rigid and require that all sperm be tested for infectious diseases using a Health Canada-approved kit. That, combined with the 2004 Assisted Human Reproduction Act—which made it illegal, among other things, to pay a man for his sperm—has made it difficult to bring in a diverse amount of sperm.
This year, Health Canada announced that as of Feb. 4, 2020, the safety requirements for sperm donation in Canada will be updated. Sperm banks exporting to the country will no longer have to use Health-Canada approved test kits—under the new rules, they can be cleared by the U.S. Food and Drug Administration (FDA).
Whether gay men will still be able to donate sperm is another question. The ban on MSM donors dates back to the mid-1980s. In a piece for Xtra earlier this year, Alison Motluk spoke to queer parents about what the new regulations mean for their families.
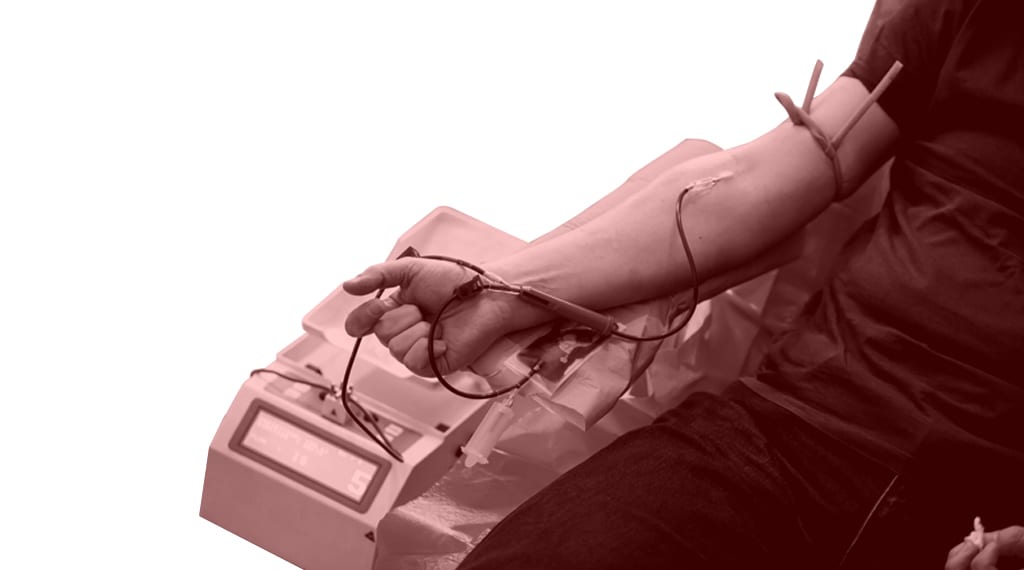
Canadian blood donation deferral drops to three months
As of June 3, 2019, the deferral period for men who have sex with men (MSM) dropped from one year down to three months after the federal Liberal government’s 2017 commitment to spend $3 million researching whether the blood ban was necessary. Health Canada announced that the recent decision was based on scientific data that shows reducing the wait times for MSM donors in 2013 and 2016 did not result in an increase of HIV-positive blood donations.
Two-Spirit, queer and trans people are included in the Missing and Murdered Indigenous Women and Girls Report (MMIWG) in Canada
The National Inquiry into Missing and Murdered Indigenous Women and Girls released its final report this year and it painted a bleak picture. The inquiry found that Two-Spirit and LGBTQ people experience colonial violence and oppression in a similar way to Indigenous women and girls. (To put that into perspective: Indigenous women and girls are 12 times more likely to face violence than non-Indigenous women, with a homicide rate seven times higher than non-Indigenous women.)
The report adds that Two-Spirit and queer Indigenous people face even more barriers than Indigenous women and girls in areas such as healthcare, child welfare, and access to justice and police because these institutions are rooted in transphobia and homophobia. Cameron Perrier further breaks down the report in his analysis of Two-Spirit and queer Indigenous people’s well-being.
Global rise in STIs
It was the year of sexually transmitted infections (STIs). The World Health Organization reported that more than one million new cases of four specific sexually transmitted infections are contracted every day: Those include chlamydia, gonorrhea, trichomoniasis and syphilis. Three kinds of STIs have hit an all-time high in the U.S., and in Canada, cases of syphilis have skyrocketed across Alberta which hasn’t seen an outbreak like this in decades.
These STIs are curable, but new, antibiotic-resistant strains—like super gonorrhoea and even some UTIs—are becoming drug-resistant. Researchers at the University of Washington have also found a new, drug-resistant bacteria among men who have sex with men which can threaten the immune system.
A decrease in condom use is being cited as one likely reason for the increase in STIs—another possible cause is stigma. LGBTQ2 people already struggle to find affirming healthcare providers, and lesbian, bisexual and queer women are also at a higher risk of STIs and HPV because of a widespread myth that they don’t need to be tested. (Read our feature on the dental dam and why it needs to make a comeback.) Trans men have a higher rate of inadequate pap testing, which puts them more at risk for infection. Interested in knowing more about pap tests and vaginal health? Dr. Jen Gunter, author of The Vagina Bible, breaks down myths about the vagina in our two-part series.
LGBTQ2 people in Canada smoke more than others
Research has found that tobacco use is much higher for LGBTQ2 people compared to the rest of the population. While about 15 percent of Canadians smoke, that rate is estimated to be between 24 and 41 percent for LGBTQ2 people—and those numbers could be even higher.
Canada’s Tobacco Strategy, which launched in 2018 to reduce overall smoking rates to less than five percent by 2035, says it specifically targets LGBTQ2 communities for intervention but didn’t specify how stigma, homophobia and transphobia play a role in the increased smoking rates found in the queer community. Brianna Sharpe’s feature explores the factors that contribute to LGBTQ2 tobacco use.
Largest surveys of Black queer, trans and gender non-binary Americans released
The Black Census is the largest survey of its kind conducted in the U.S. since the Reconstruction era. Led by Black Futures Lab, which was established by Black Lives Matter co-founder Alicia Garza, it partnered with dozens of organizations around the country to survey more than 31,000 Black people. One survey was devoted to LGB+ people, and another, separate report exploring the distinct concerns and experiences of respondents who identify as transgender, gender non-conforming or identify their gender as “different” than male or female was recently released.
Some takeaways: Low wages, lack of affordable healthcare and lack of affordable housing were identified as major concerns for all genders; lesbians are more likely to support marriage rights than other Black queer people; bisexual respondents and those who identify as “other” are most likely to experience rising college costs and transgender and gender non-conforming or non-binary respondents are more likely to live in extremely economically precarious lives.
Trans women of colour reveal their experience as teenagers
Researchers in the U.S. have completed what they call a “first of its kind” study into the adolescent experiences of young transgender women of colour.
Some takeaways: Latinx women were among the youngest to become self-aware that they are trans (around age nine), and Black women were the oldest (around age 11); Black and Latinx women begin disclosing their trans identity to others between the ages of 13 and 15, while white transgender women did not do so until around 17; Black trans women begin taking hormones at 19, while white trans women, the latest, begin at 22.
The results of the study illustrate the need for more support systems for young trans women — especially earlier in life. This is particularly true for young trans women of colour who come out and reach sexual developmental milestones much earlier than their white counterparts. Along with these factors and racial and gender discrimination, the study suggests more social and sexual health supports for young trans women of colour at an early age.

Canadian government provides a detailed look at LGBTQ2 health
The House of Commons Standing Committee on Health released ground-breaking recommendations that, if implemented, could radically improve the health of LGBTQ2 communities across Canada.
The report provides an overview of the current state of LGBTQ2 health—and it doesn’t paint a pretty picture when it comes to substance abuse or physical, mental and sexual health. The committee blames the social, legal and economic factors that limit access to health and wellness care for queer, trans and gender nonconforming people. Fae Johnstone presents nine important highlights from the report.
Bisexuals experience some of the worst health outcomes
Bisexual health—especially of bisexual women—was one of the leading topics this year (fun fact: Bisexual people make up over half of the queer community!). As more people begin to identify as bisexual than ever before—many of them female-identified—why are their health outcomes so bad, and what’s being done to improve them?
Several studies paint a grim picture of bisexual women’s physical and mental health, examining how biphobia from both inside and outside the queer community contributes to their poor health. Bisexual women are more likely than lesbians to have chronic health issues, smoke cigarettes and cannabis, abuse alcohol and experience interpartner violence.
New technology offers more options for HIV-positive parents
Even among the HIV-positive and surrogacy communities, there is little knowledge about how poz men can safely father children without transmitting the virus. But sperm washing might be the answer. It’s a relatively inexpensive treatment—somewhere between $300 and $850 a pop—and involves diluting a fresh semen sample with a solution containing antibiotics and protein supplements.
All of this should make working with HIV-positive semen samples relatively straightforward (especially considering that someone with an undetectable viral load can’t transmit the virus). But Canadian Standards Association guidelines require that laboratories store semen samples from poz men in specially reinforced containers, which are costly and require additional laboratory space. Alexandra Kimball takes a deep dive into the lives of HIV-positive men who are trying to start a family.

For more health and wellness coverage, check out our “Ask an Expert” series, which tackles your burning questions about sex and reproductive health, or our “Seeing Red” series, about LGBTQ2 people and their periods. If your New Year’s resolution is to start your glow-up from the inside out, we have some great tips on how to find an LGBTQ2-affirming therapist. And if you just need a warm hug, check out our column Ask Kai: Advice for the Apocalypse.

This story is part of our Rainbow Rewind 2019 series—looking back at the past year and decade in politics, health, culture and more.


 Why you can trust Xtra
Why you can trust Xtra


